Rejection Message
NDC code [] is invalid. Procedure code <CPT> NDC code [] must be 11 digits.
Edit the procedure code under Settings > Codes > Find Procedure.
Find procedure code 'CPT' and edit the NDC and make sure it has 11 digits. Dashes (-) are ignored.
|
Rejection Details
Kareo Validation Error
This rejection indicates the claim includes a procedure (CPT/HCPCS) code with an National Drug Code (NDC) number in the incorrect format.
Note: Since claims rejected within Kareo are not forwarded to the clearinghouse, timely filing cannot be generated for the submission until validation errors have been corrected and the claim resubmitted.
|
Resolution
Follow the steps below depending on whether the National Drug Code (NDC) number was entered in the Procedure or Encounter record.
- If the NDC number was entered in the Procedure record:
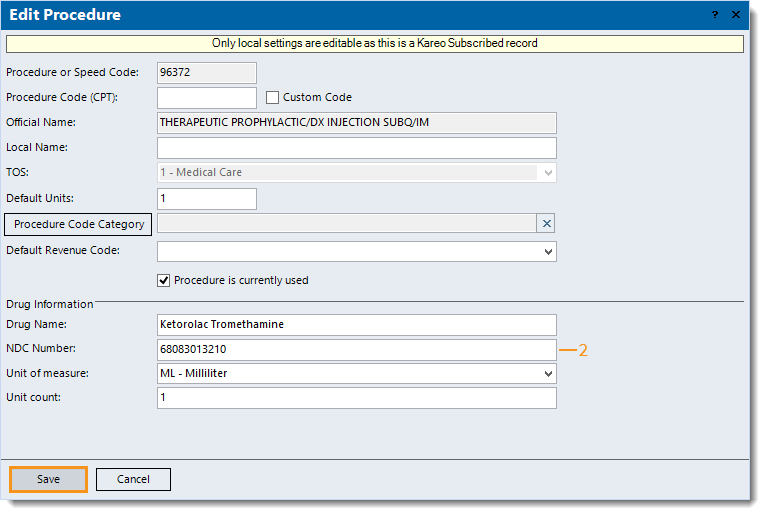
- Find and open the procedure. The Edit Procedure window opens.
- Under the Drug Information section, update the NDC Number to the correct 11-digit format (excluding hyphens).
- If required by the payer, enter additional drug information related to the NDC number.
Note: When unsure, contact the payer to verify the required drug information to prevent further claim rejections.
- Click the drop-down arrow and select the appropriate Unit of measure.
Note: The MCG and MG qualifiers are only accepted on paper claims.
- Enter the Unit count.
- Click Save.
Then, rebill and resubmit all affected claims.
|
|
- If the NDC number was entered in the Encounter record:
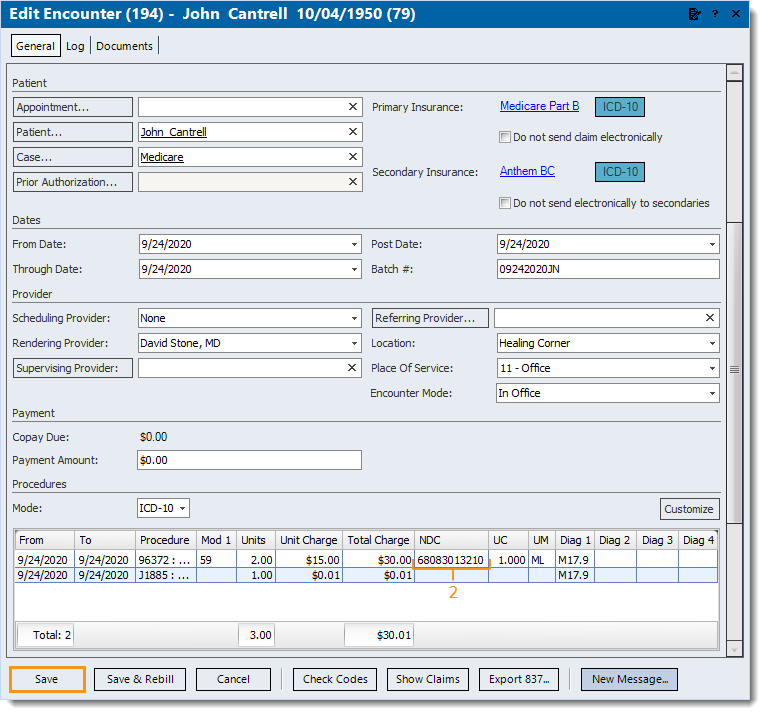
- Find and open the encounter. The Edit Encounter window opens.
- Under the NDC column of the Procedures section, update the NDC number to the correct 11-digit format (excluding hyphens).
- If the NDC column is not displayed, customize the Procedures section to add the NDC column.
- If required by the payer, update or enter additional drug information related to the NDC number.
Note: When unsure, contact the payer to verify the required drug information to prevent further claim rejections.
- UC: Enter the unit count (e.g., if 1 vial is 1 mL, the UC is 1).
- UM: Enter the unit of measure (e.g., if 1 vial is 1 mL, the UM is ML).
Note: The MCG and MG qualifiers are only accepted on paper claims.
- Click Save.
Then, rebill and resubmit all affected claims.
|
 |

