INVALID DIAGNOSIS CODE TYPE - EXPECTED VALUE IS ICD-9
|
Rejection Message INVALID DIAGNOSIS CODE TYPE - EXPECTED VALUE IS ICD-9 |
|
|
Rejection Details Claims submitted with dates of service prior to 10/1/2015 must contain ICD-9 codes. |
|
|
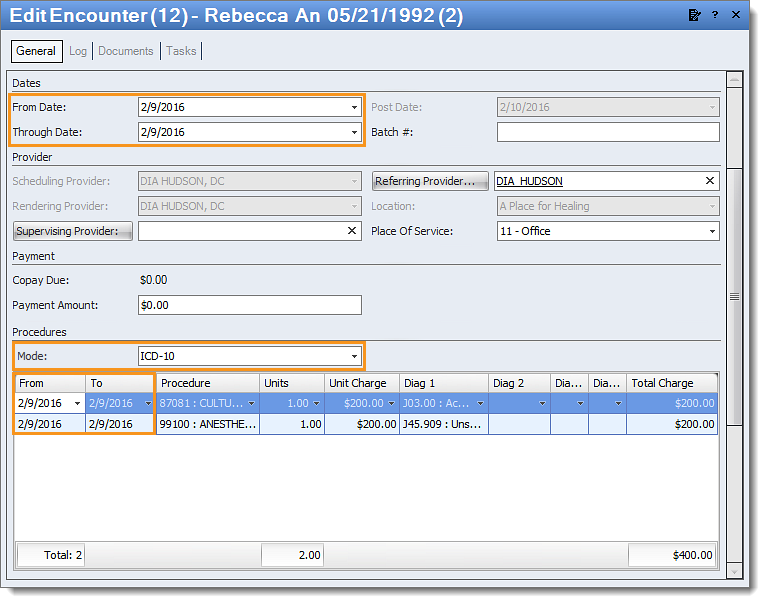
Resolution Follow the instructions below to verify the dates of service and mode on the encounter is correct:
Then, rebill and resubmit all affected claims. |
 |